We are a multi-hospital healthcare network that partnered with Viston to reduce claim denials, speed up prior authorizations, and improve patient support without compromising PHI security.
Business challenge
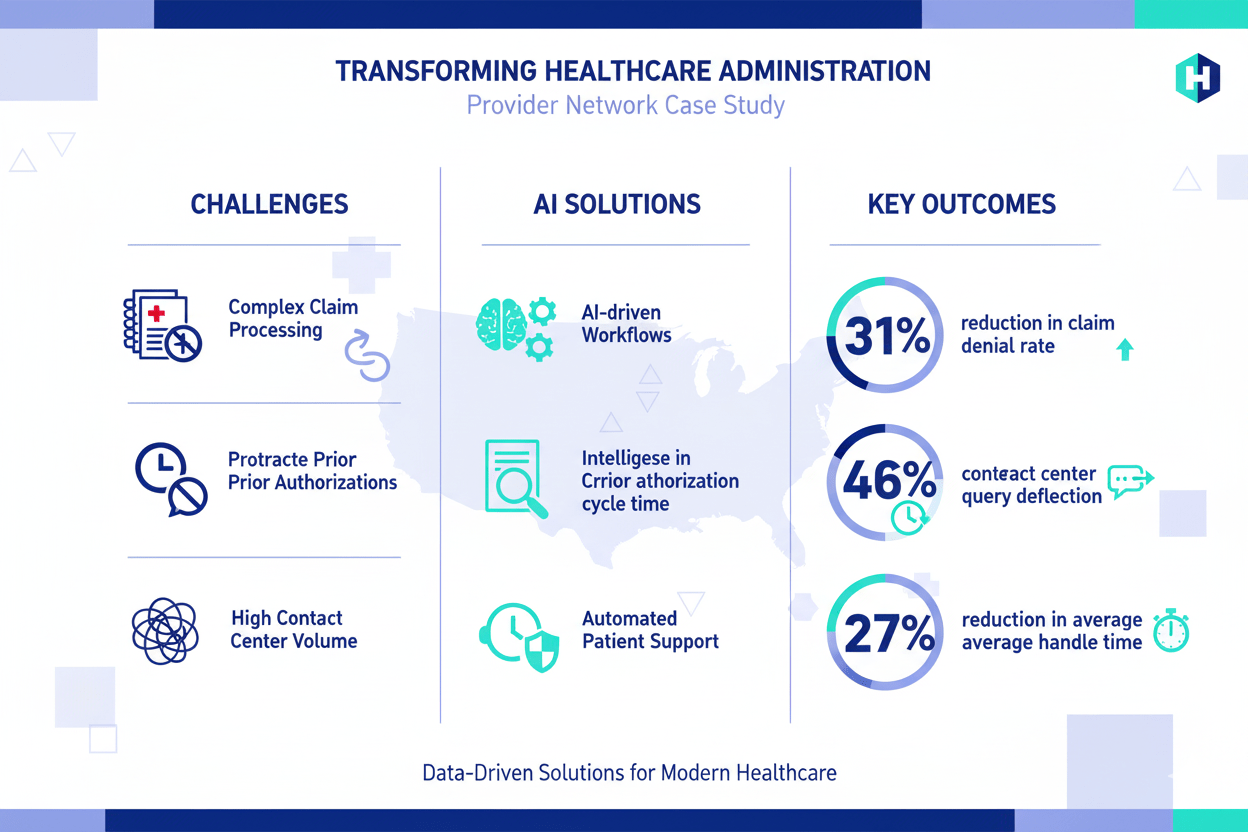
Claim denial rate at 12.8%, long prior authorization cycles (72 hours median), and 27% of patient inquiries waiting over 10 minutes for resolution.
Contact center average handle time was 8.6 minutes with inconsistent documentation quality.
Our approach and solution
Viston conducted a HIPAA-first data audit, signed a BAA, and deployed an isolated Azure tenant with PHI redaction and FHIR-first integrations.
Delivered three workstreams:
Medical Coding Copilot with RAG over payer rules, ICD-10/HCPCS, and our historical approvals.
Prior-Auth Summarizer that compiles clinical notes and guidelines into payer-ready packets.
Patient Support Assistant for scheduling, benefits eligibility, and prep instructions, escalated via human-in-the-loop.
AI applications and benefits delivered
NLP/RAG for clinical summarization, denial reason prediction, and intent classification in patient queries.
Benefits: fewer denials, faster authorizations, 24/7 triage with safe handoffs, and improved documentation consistency.
Cost of implementation
USD 165,000 inclusive of cloud, licenses, security hardening, and 6 months of MLOps support.
Time to implement
14 weeks to pilot, 10 weeks to scale across 3 hospitals.
Tools and technologies used
Azure OpenAI (GPT-4 class), Azure Cognitive Search, FHIR server, Databricks, LangChain, n8n for workflow automation, Power BI, Key Vault, Private Link.
Quantitative outcomes
Claim denial rate reduced by 31% (to 8.8%).
Prior-auth median cycle time reduced by 46% (to 39 hours).
Contact center deflection of routine queries: 38%.
Average handle time reduced by 27% (to 6.3 minutes).
3.2x ROI within 10 months.
Key performance indicators (KPIs) tracked
Denial rate, prior-auth turnaround time, AHT, first-contact resolution, CSAT, PHI leakage incidents, model accuracy on medical intents.
Pre- and post-implementation metrics
Denials: 12.8% → 8.8%.
Prior-auth time: 72h → 39h.
AHT: 8.6m → 6.3m.
CSAT: 4.1/5 → 4.5/5.
Stakeholder quotes or testimonials
“Viston gave our teams superpowers while meeting our HIPAA bar. The coding copilot alone paid for itself in under a year.” — VP, Revenue Cycle
Regulatory or compliance considerations
HIPAA, SOC 2 Type II, BAA in place, PHI redaction, audit logging, least-privilege access, model governance with prompt/response retention policies.